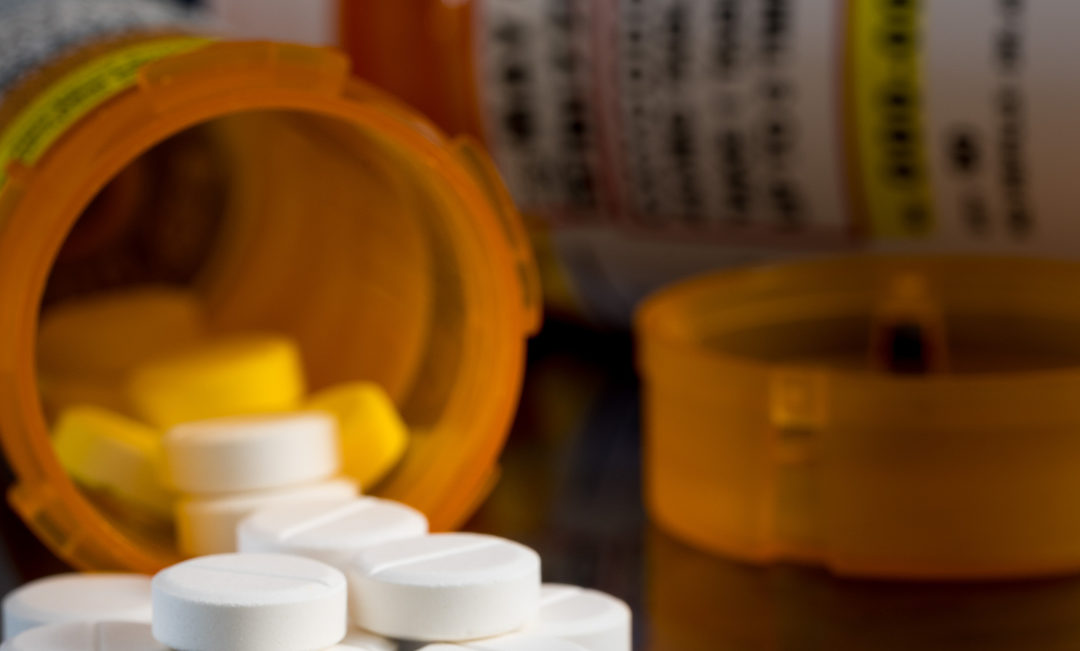
Opioids, Chronic Pain, and Addiction
There remains a robust debate about the use of opioids for the treatment of chronic pain. According to scientific research, much of it released within the last decade, the risk of addiction, side effects, and/or overdosing outweigh the benefits of taking opioids for chronic pain unrelated to cancer (e.g., for lower back pain or migraines).
In a 2019 study published by Mayo Clinic Proceedings, the authors write, “In the 1990s, a confluence of economic, medical, and governmental factors coalesced into a mutual driver of widespread prescription opioid use for chronic pain. The havoc wrought by this shift in prescribing practices ushered in the most devastating addiction crisis in U.S. history.”
The study’s authors cite statistics showing that in 2018 almost 200 people in the United States died each day from a drug overdose.
“Opioids were responsible for approximately two-thirds of the deaths,” they write.
Long-Term Effects
Additional research into the long-term effects of opioids has altered the medical landscape regarding opioids. For example, the American Academy of Neurology has called for closer tracking of opioid treatment. They’ve also encouraged studies into alternative approaches to the treatment of chronic pain.
Even in cases in which opioids have proven beneficial to a specific patient, experts recommend keeping a close watch on dosage. Patients also need to be screened for substance abuse, depression, and general misuse of this powerful narcotic.
This isn’t the first time such a discovery has been made, but it has renewed the push for more restraint when it comes to prescribing opioids.
A Research-Based Approach
While not the first group to argue this point, it is the first time guidelines based on research have been put on the table. The researchers lay out in a clear guide who might benefit the most (and least) from long-term opioid use and exactly what a physician should do when tracking these prescriptions.
If adopted, new tactics for managing codeine, methadone, hydrocodone, morphine, and oxycodone may follow.
The official position of the American Academy of Neurology also encourages doctors to work closely with officials to shift outdated policies from the 1990s, which made it fairly common to prescribe opioid-based pain medicines.
The research suggests adding stronger monitoring programs which will include a virtual database so doctors can instantly see what drugs a patient has been prescribed in the past.
As reported by the Los Angeles Times in 2014, it’s noted that such systems are “currently underfunded, underutilized and not interoperable across state lines or healthcare systems.”
High Tolerance, High Risks?
Just like with any drug, a person’s tolerance goes up the more they use it. This means they’ll need higher and higher doses to get the same painkilling result. This leads to misuse, abuse, and a higher chance of overdosing.
Those most vulnerable to overdosing are aged 35 to 54. In recent years, drug overdoses have killed more people than guns and traffic accidents.
Research has also shown that people who take opioids for a minimum of three months (as a temporary prescription) continue to do so for at least five years. During this time, most of the prescriptions increase in strength, and yet the results remain the same in the patient.
Moves to Make
Along with the improved screening, it’s recommended that doctors draft so-called “opioid treatment agreements” with their patients. These outline the roles of patients with chronic pain and primary care doctors tasked with treating pain symptoms.
Whenever a dosage increase is on the table, the patient’s function level should also be noted. If the opioids aren’t working, perhaps a pain specialist is a better answer than higher doses.
The ultimate goal is pain management without such narcotics for long-term care — especially considering the findings from these and other continuing studies.
Pain medications, pain relievers — both short-term and long-acting — have their place in pain treatments. Finding a healthy and stable balance between pain relief, opioid therapy, and overall health care will surely be the topic of continued focus from medical professionals. Contact MBA Medical the medical billing experts today!