
by Web Master | Apr 17, 2024 | Blog
A Comprehensive Guide to RVU Medical Billing In the complex world of medical billing, understanding the ins and outs of Relative Value Units (RVUs) is crucial for medical billers. RVUs play a pivotal role in determining reimbursement rates for medical services, but...

by Web Master | Apr 11, 2024 | Blog, Medical Practice Management, News
In February, one of the largest clearinghouses of medical information–patients and providers alike–fell victim to a cyber attack. Change Healthcare, a division of Optum under the UnitedHealth Group umbrella, is responsible for an incredible amount of data that changes...
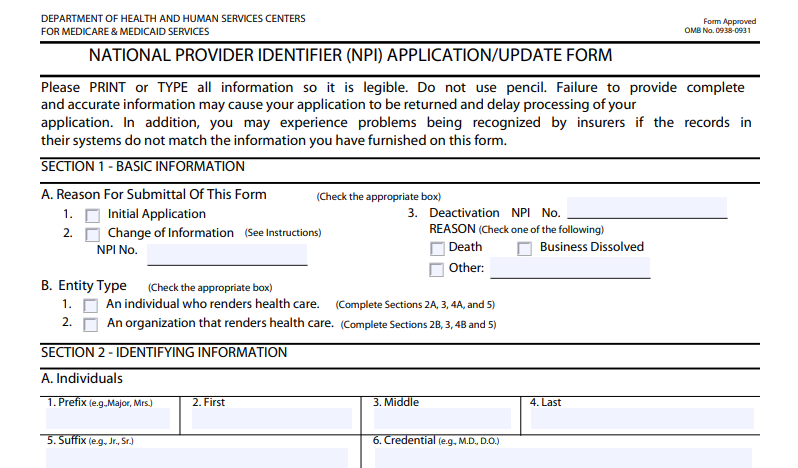

by Web Master | Mar 20, 2024 | Blog
No matter if you’re a surgeon, nurse, pharmacist, or massage therapist, you got into the profession because you want to help people. This can mean helping your patients fight disease, fix broken bones, make them more comfortable, or any one of thousands of other...

by Web Master | Mar 13, 2024 | Blog
Are you interested in saving money? Or, better yet, are you interested in making money? In today’s healthcare landscape, where every dollar counts and compliance is non-negotiable, mastering your revenue cycle is not just a choice; it’s a prescription for...
by Web Master | Mar 6, 2024 | Blog
Tell us if this sounds familiar to you as a patient: You went to your healthcare specialist for a regular checkup. At the end of the month, you’re given a bill for unpaid services that seem a little extravagant for a normal office visit to your doctor. If this has...






